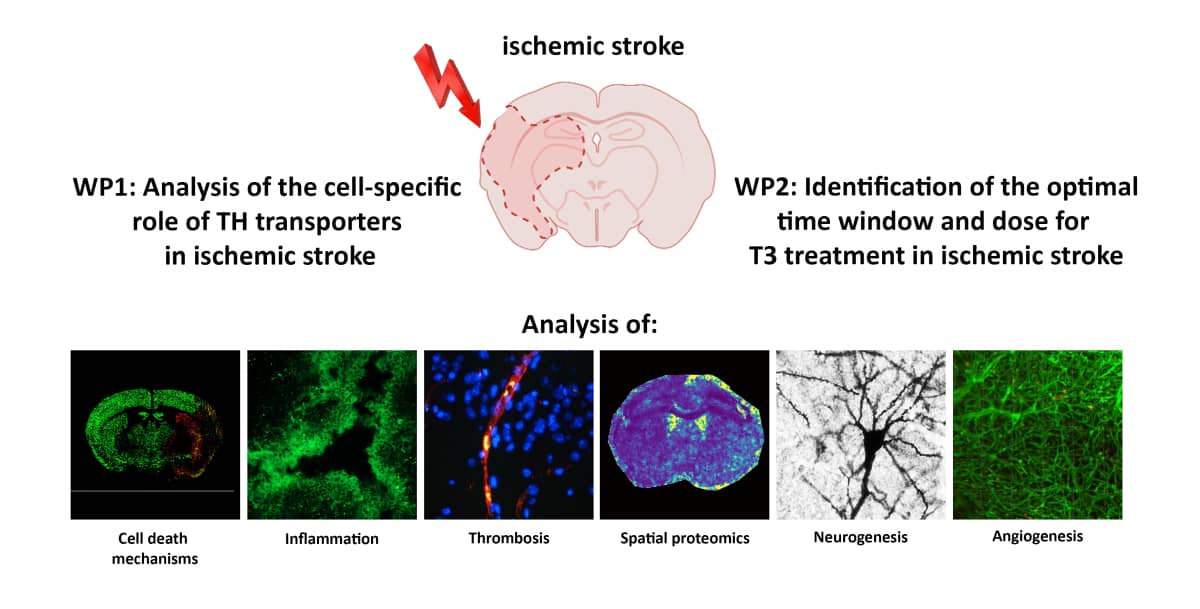
Local TH transport and action in ischaemic brain injury
Dr. Friederike Langhauser, Prof. Dr. med. PhD Dagmar Führer & Prof. Dr. med. Christoph Kleinschnitz
Aim of this project is to clarify the time- and cell-specific requirements of TH transport and action for improved outcome in ischaemic brain injury. Cell-specific TH transporter KO mice will be analysed in the experimental stroke model of transient middle cerebral artery occlusion (MCAO) to elucidate the role of TH transport in different cell-types of the blood brain barrier. Treatment with T3 at different dosages and time points will be used to identify the optimal conditions for intervention. The impact of TH on stroke outcome will be analysed by functional, morphological and imaging techniques, e.g. light sheet microscopy and spatial proteomics.
Further Information
Selected Publications
Calcium-dependent blood-brain barrier breakdown by NOX5 limits postreperfusion benefit in stroke.
Casas AI, Kleikers PW, Geuss E, Langhauser F, Adler T, Busch DH, Gailus-Durner V, de Angelis MH, Egea J, Lopez MG, Kleinschnitz C, Schmidt HH.
2019. J Clin Invest 129(4):1772-1778. doi: 10.1172/JCI124283
A diseasome cluster-based drug repurposing of soluble guanylate cyclase activators from smooth muscle relaxation to direct neuroprotection.
Langhauser F, Casas AI, Dao VT, Guney E, Menche J, Geuss E, Kleikers PWM, López MG, Barabási AL, Kleinschnitz C, Schmidt HHHW.
2018. NPJ Syst Biol Appl 4:8. doi: 10.1038/s41540-017-0039-7
Blocking of α4 integrin does not protect from acute ischemic stroke in mice.
Langhauser F, Kraft P, Göb E, Leinweber J, Schuhmann MK, Lorenz K, Gelderblom M, Bittner S, Meuth SG, Wiendl H, Magnus T, Kleinschnitz C.
2014. Stroke 45(6):1799-806. doi: 10.1161/STROKEAHA.114.005000
Stroke-induced chronic systolic dysfunction driven by sympathetic overactivity.
Bieber M, Werner RA, Tanai E, Hofmann U, Higuchi T, Schuh K, Heuschmann PU, Frantz S, Ritter O, Kraft P, Kleinschnitz C.
2017. Ann Neurol 82(5):729-743. doi: 10.1002/ana.25073
Blood coagulation factor XII drives adaptive immunity during neuroinflammation via CD87-mediated modulation of dendritic cells.
Göbel K, Pankratz S, Asaridou CM, Herrmann AM, Bittner S, Merker M, Ruck T, Glumm S, Langhauser F, Kraft P, Krug TF, Breuer J, Herold M, Gross CC, Beckmann D, Korb-Pap A, Schuhmann MK, Kuerten S, Mitroulis I, Ruppert C, Nolte MW, Panousis C, Klotz L, Kehrel B, Korn T, Langer HF, Pap T, Nieswandt B, Wiendl H, Chavakis T, Kleinschnitz C and Meuth SG.
2016. Nat Commun 7:11626. doi: 10.1038/ncomms11626
Endothelial TWIK-related potassium channel-1 (TREK1) regulates immune-cell trafficking into the CNS.
Bittner S, Ruck T, Schuhmann MK, Herrmann AM, Moha ou Maati H, Bobak N, Göbel K, Langhauser F, Stegner D, Ehling P, Borsotto M, Pape HC, Nieswandt B, Kleinschnitz C, Heurteaux C, Galla HJ, Budde T, Wiendl H, Meuth SG.
2013. Nat Med 19(9):1161-5. doi: 10.1038/nm.3303
Regulatory T cells are strong promoters of acute ischemic stroke in mice by inducing dysfunction of the cerebral microvasculature.
Kleinschnitz C, Kraft P, Dreykluft A, Hagedorn I, Göbel K, Schuhmann MK, Langhauser F, Helluy X, Schwarz T, Bittner S, Mayer CT, Brede M, Varallyay C, Pham M, Bendszus M, Jakob P, Magnus T, Meuth SG, Iwakura Y, Zernecke A, Sparwasser T, Nieswandt B, Stoll G and Wiendl H.
2013. Blood 121(4):679-91. doi: 10.1182/blood-2012-04-426734
Kininogen deficiency protects from ischemic neurodegeneration in mice by reducing thrombosis, blood-brain barrier damage, and inflammation.
Langhauser F, Göb E, Kraft P, Geis C, Schmitt J, Brede M, Göbel K, Helluy X, Pham M, Bendszus M, Jakob P, Stoll G, Meuth SG, Nieswandt B, McCrae KR, Kleinschnitz C.
2012. Blood 120(19):4082-92. doi: 10.1182/blood-2012-06-440057







